Abstract
Facial palsy, or weakness of the facial muscles, arises from injury to the facial nerve and can lead to debilitating morbidity by affecting facial expression, speech, and daily activities. Playing a wind instrument, such as the saxophone, requires formation of an airtight seal with the instrument's mouthpiece through a coordinated effort of facial muscles known as embouchure. Consequently, facial palsy can impair a musician's ability to play a wind instrument. To address this functional disability, we present a novel three dimensional (3D) printed embouchure-assistive device designed for application in saxophone players with facial palsy. Quantitative and qualitative metrics were recorded, demonstrating improved duration of note sustain, increased mean air pressure within the mouthpiece during play, and subjectively improved patient comfort and overall tone quality with use of the device. We also include design iterations of the prototype device as they may serve as a template for broader applications in musicians with facial palsy.
Keywords
1. Introduction
Facial palsy, or weakness of the facial muscles, arises from injury or insult to the facial nerve. Common etiologies include idiopathic Bell's Palsy, neoplastic, traumatic, stroke, congenital, or iatrogenic causes[1]. While many cases of facial paralysis or weakness are transient and self-resolving, patients with permanent dysfunction often require surgical intervention to reestablish facial muscle function[2]. Facial palsy is associated with significant morbidity, including incomplete eyelid closure leading to corneal injury, oral incompetence, difficulty with producing labial consonants such as /b/ and /p/, and significant psychosocial impact resulting in reduced quality of life and depression[3-5]. Despite the extensive body of research on impacts of facial palsy, one often overlooked matter is the effect it may have on music production.
To play a woodwind instrument such as the clarinet, saxophone, or bassoon, one must create an airtight seal between their lips, tongue, and the instrument's mouthpiece. Sound is produced while blowing via a complex coordinated movement of the throat, tongue, jaw, teeth, lips, and cheeks, known cumulatively as an embouchure[6]. Electromyography of the embouchure-forming facial muscle groups have revealed that muscles involved in airflow emission control and articulation (i.e. buccinator and mylohyoid) are most active during woodwind playing, followed by muscles that stabilize the mouthpiece (i.e. masseter, mentalis, orbicularis oris, depressor oris)[2]. Patients with facial palsy may have limited or absent function of these muscles of embouchure[6]. The loss of muscle tone and function prevents the player from applying sufficient soft tissue pressure upon the instrument mouthpiece, resulting in excessive air leakage. This drops the intra-instrument airflow below the threshold needed to produce a high-quality tone and sustained sound.
The impact of embouchure dysfunction on the career and life of a professional musician can be profound. A survey of musicians with focal dystonia of the embouchure, a separate but similar condition involving dysfunction and weakness of the oral facial muscles, revealed that 50% stopped playing altogether after onset of impairment[7]. Given the significant and specific impact that facial palsy can have upon woodwind musicians, the primary objective of this study was to develop an open-access, three dimensiona (3D) printed embouchure-assistive device to help patients with facial palsy regain the ability to play the saxophone. Secondary objectives included overall cost, reproducibility, device stability, musician comfort, and universality to accommodate a wide variety of saxophone mouthpieces.
2. Case
A 62-year-old man with over 20 years of experience playing the saxophone, clarinet, and flute at a semi-professional level, presented to a Head & Neck Surgery clinic in the community with several months of left jaw claudication. Workup revealed a 1.8 cm well-circumscribed tumor within the left parotid gland. Informed consent was obtained, and the patient underwent a planned left parotidectomy. Intraoperatively, frozen sections revealed malignancy and the tumor was found to be entirely encasing the facial nerve, so resection was aborted. The final pathology confirmed a diagnosis of adenoid cystic carcinoma, and the patient was referred to our academic and tertiary care center. Informed consent was obtained, and he subsequently underwent completion parotidectomy with facial nerve sacrifice and ipsilateral neck dissection with concurrent nerve repair and dynamic reanimation procedure. A 7 cm segment of facial nerve was excised up to the main trunk as it exited the stylomastoid foramen. Nerve repair included sural nerve harvest and cable graft to the temporal, zygomatic, buccal, and mandibular branches of the facial nerve. Dynamic reanimation involved nerve transfer (nerve to masseter (V3) to smile branches of VII). There were no immediate complications. He completed adjuvant proton therapy without sign of recurrence to date.
In the three years since completing treatment, nerve rehabilitation was partially successful. The left-sided facial nerve function regained modest tone in the eyelid, cheek, and oral commissure with restricted motion and weak effort of these muscle groups along with moderate mentalis and depressor labii synkinesis, as shown in Figure 1. The patient reported that his left-sided facial palsy impaired his ability to effectively play his woodwind instruments due to difficulty forming an air-tight seal with the mouthpiece.

Figure 1. Patient with left sided facial palsy (prior to onset of partial recovery). Photographs published with permission from patient.
3. Methods
3.1 Measurements
Objective measurements of facial asymmetry and degree of facial palsy were obtained with clinical photographs and use of Emotrics software, as shown in Figure 2. A 3D scan of the patient's face was generated with the app, KIRI Engine (KIRI Innovations Science and Technology Inc, Ancaster, Ontario, Canada L9K 1P8) for digital prototyping, as shown in Figure 3. Scans were used to obtain measurements of the lip, oral commissure, and the angle of curvature of the left side of the patients face. To identify areas of leakage and weakness in the formation of his embouchure, molds were taken of the patient's embouchure using SDent® silicone impression putty (SDent, Shanghai S&D International Trade Co., Ltd., Shanghai, China). Molds were hand-pressed over the exterior of the patient's mouth, first with lips closed shut together and then with lips closed around an inserted saxophone mouthpiece. KIRI Engine was also used to make the 3D digital models of the dental molds in Figure 4.
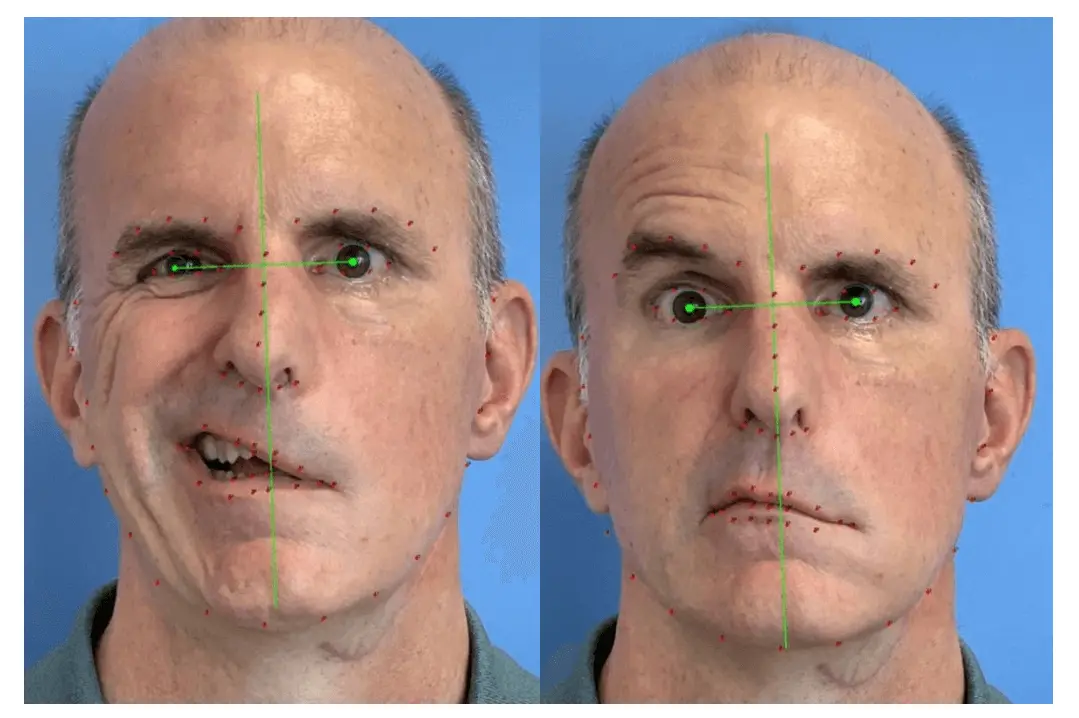
Figure 2. The extent of left facial palsy was quantified using Emotrics software[8]. Unmatched strength from healthy muscles on the patient's right create a right midline shift of his mouth. Photographs published with permission from patient.

Figure 3. 3D digital model of the patient's face and embouchure with mouthpiece inserted, created with KIRI Engine. Photographs published with permission from patient. 3D: three dimensional.
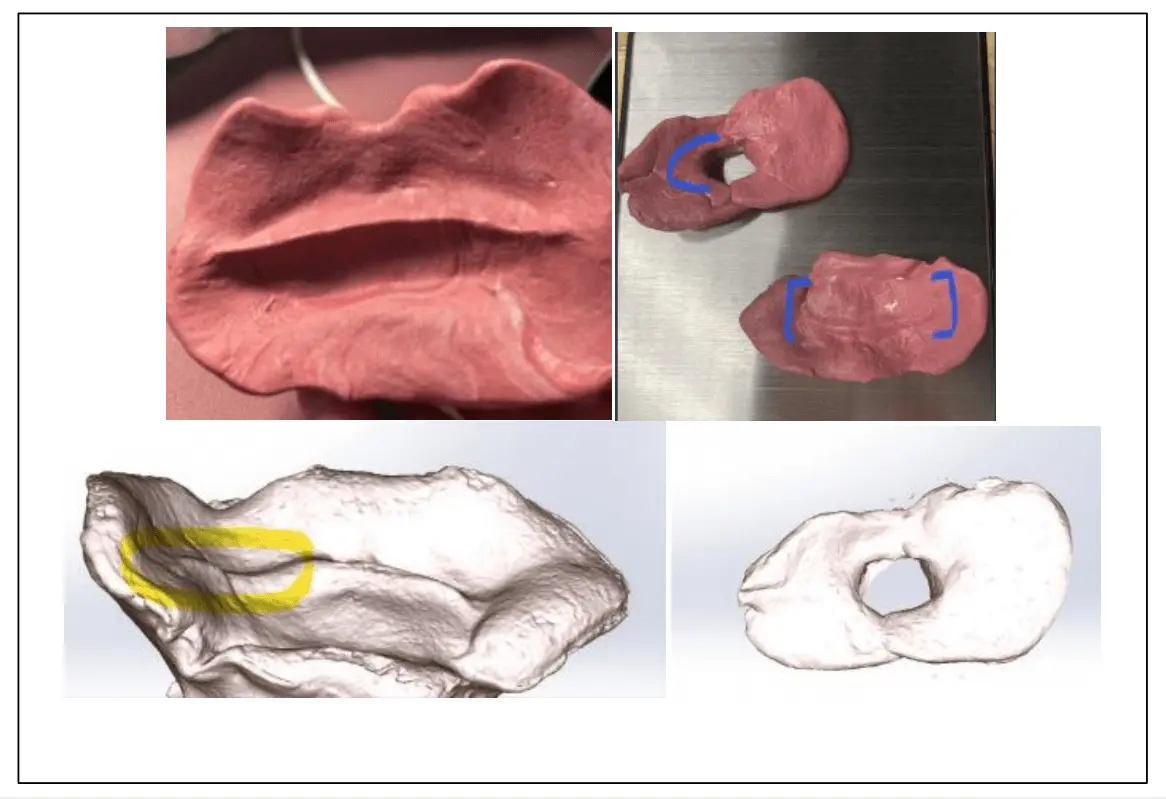
Figure 4. Images depicting dental molds and 3D digital models of the molds used to detect areas of leakage and weakness in the patient's embouchure. 3D: three dimensional.
3.2 Materials
Materials were selected for properties of accessibility (cost), strength, comfort, and biocompatibility in order to build a cost-effective but high-quality device that properly supported muscles of the embouchure and rested against the patient's skin with maximal comfort over time. To ensure accessibility and reproducibility of the device, the main structural material was selected from an array of materials that can be readily printed using a fused deposition modeling (FDM) 3D printer, one of the cheapest and most available printers on the market. Among materials that are compatible with FDM 3D printers, thermoplastic polyurethane (TPU) was found to be a widely available biomedical grade common rubber material that possessed an ideal blend of cost-efficiency, strength, and flexibility. Copper 3D MD Flex TPU was specifically selected for use due to its antimicrobial action and FDA approval for food handling and medical usage (Copper 3D, Santiago, Chile). Copper 3D MD Flex TPU has a Shore A hardness of 98A, which offers some flexibility without sacrificing durability (Copper 3D, Santiago, Chile). Tensile modulus, a mechanical property defined as a ratio of tensile stress (force per unit area) to its strain (relative deformation), was used to determine if the selected material was stiff enough to maintain shape against force exerted when the patient blows into the mouthpiece. Copper 3D MD Flex TPU has a tensile modulus of 150 MPa (Copper 3D, Santiago, Chile), far above the blowing pressure of reed instruments around 0.5 kPa relative to atmospheric pressure[9]. Early prototypes produced using TPU alone were uncomfortable on the patient's face, so subsequent prototypes were dipped in medical grade silicone to comfortably interface with the patient's skin and mouth. From a medical standpoint, silicone padding has had documented benefits in preventing the development of pressure ulcers, which are wounds which develop due to prolonged exposure of skin to pressure or friction[10]. EcoFlex® silicone was chosen due to its documented textural similarities to dermis, strength, elasticity, and its usage in the development of prosthetics[11-13]. By combining a stiff but flexible Copperflex 3D MD TPU inner structure with softer EcoFlex silicone as an outside layer, the device was able to be made both strong enough to withstand force and deformation and soft enough to interface comfortably and safely with the patients face. Digital designs were made through computer aided design (CAD) with the software program Solid Works (Dassault Systemes SolidWorks Corp., Waltham MA, USA)[14].
3.3 Design
Several prototypes were modeled to fit around a tenor saxophone mouthpiece; subsequent iterations were tested toward improving the patient's comfort and their effectiveness in forming an oral seal with the instrument mouthpiece (Table S1).
The final designed device utilizes a rigid, 3D printed TPU construction with a soft silicone overlay. Early methods of device design involved dipping the TPU structure thrice into silicone, but this did not produce an external silicone layer thick enough to offer optimal comfort or deform with the natural variations and curvature of the patient's dynamic embouchure to form a proper seal. Instead, a thick silicone cushion was created using a custom mold and was adhered to the surface of the TPU structure that interfaced with the patient's face. The silicone cushion adapted to fluidly fill unpredictable dips and curves in the patient's changing embouchure, and as such this design yielded the greatest subjective comfort for the patient and the best air seal. The rigid TPU structure slides over the saxophone mouthpiece and is secured with a hose clamp to resist the counterpressure of the user's face while playing. Zip-ties and Loctite adhesive were used to attach a thick, malleable EcoFlex silicone 5 mm overlay to the TPU structure, as shown in Figure 5. One zip-tie was fastened at the device's lateral end to secure the silicone pad to the TPU structure, while the second zip-tie fastened around the TPU structure but beneath the silicone pad, allowing it to slide laterally and adjust the angle of the silicone pad. The thick silicone interface lay flush against the patient's skin and its precise angle was adjusted with the zi p-ties by the patient to fill the gaps in his embouchure. The final 3D printed device prototype CAD Solid Works file is available for free-access download, reproduction and validation (File S1).
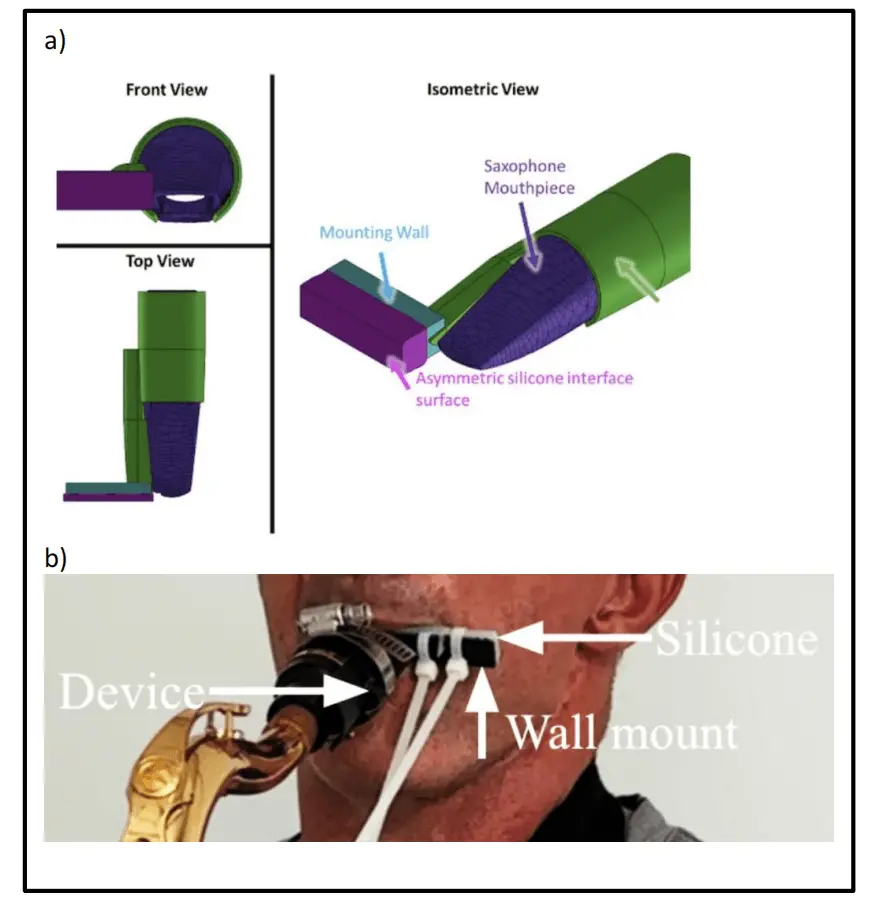
Figure 5. Embouchure assist device. a) Final device digital design: device sleeve (green), mounting wall (blue), silicone interface (magenta), saxophone mouthpiece (dark purple); b) final TPU construction to fit saxophone mouthpiece, with overlying thick malleable EcoFlex silicone pad facial piece, secured with zip ties, allowing for the patient to form a customized embouchure seal. TPU: thermoplastic polyurethane.
3.4 Device efficacy
The device's efficacy was assessed by measuring duration of note sustain and measurement of air pressure within the instrument. Data was obtained using the patient's tenor saxophone, with and without the embouchure-assistive device. An Arduino-compatible silicon piezoresistive NXP MPX10DP pressure sensor was secured to a tenor saxophone mouthpiece with leads placed at the proximal and distal ends (NXP Semiconductors, Eindhoven, The Netherlands). To accommodate the sensor, the mouthpiece was drilled to accept two 1/8" diameter tubes in the resonance chamber, which were inserted and secured flush with the inner wall of the mouthpiece bore. Short lengths of hose were connected between these tubes and the inlets on the NXP MPX10DP pressure sensor. The segments of connected hose were designed to be as short as possible to minimally interfere with the natural airflow through the mouthpiece. In piezoresistive sensors, four resistors are placed on a silicon diaphragm in order to measure the result of strain or physical pressure applied upon them. Any change in resistance is converted through a Wheatstone bridge circuit into an output voltage[15]. This design served as a compact, accurate, and affordable sensor with high resolution digital output, as shown in Figure 6. Initial calibration of the pressure sensor was performed at known pressures (5, 10 and 15 kPa) prior to integration into the saxophone mouthpiece. Once the pressure sensor was installed, absolute pressure values inside the mouthpiece could not be validated with means available. However, as the intent was to compare quantitative changes in intra-mouthpiece air pressure with and without the device, consistency in pressure measurement methodology between trials with and without the device was more critical than the absolute pressure value in the mouthpiece itself.
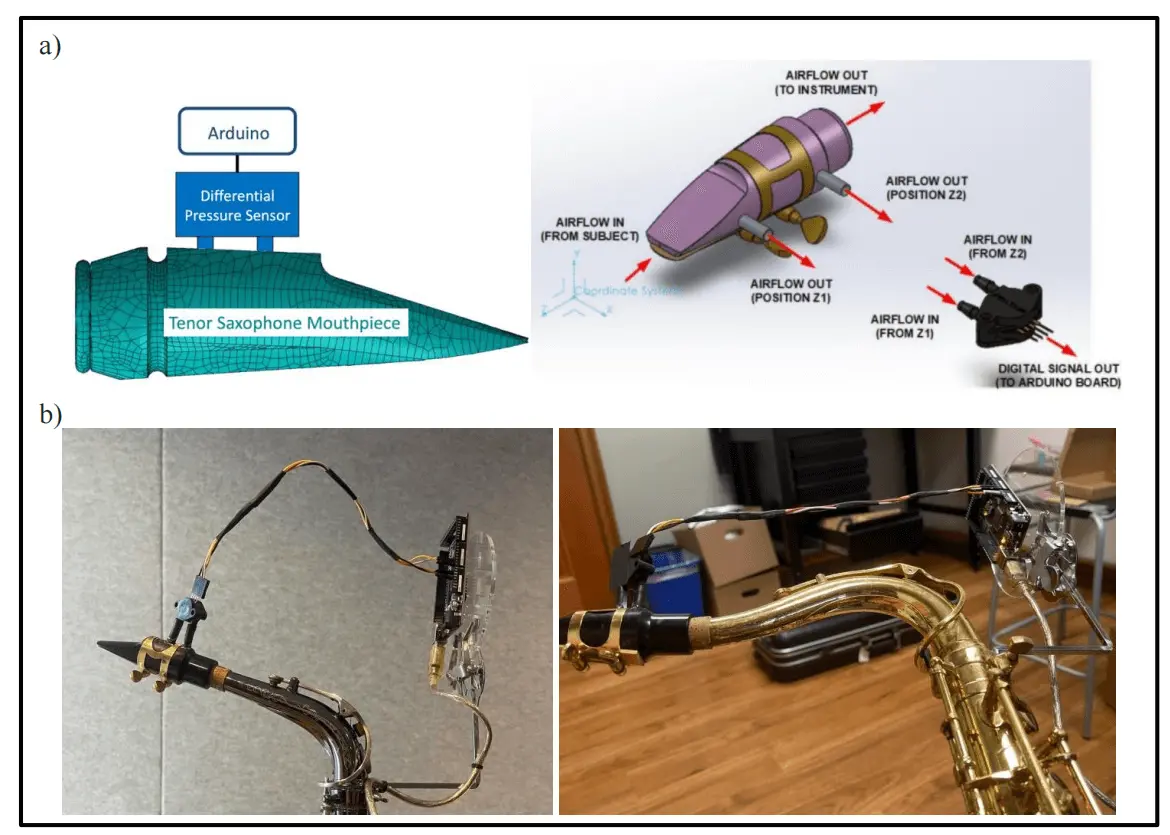
Figure 6. a) Diagram of the air pressure sensor connected to the Arduino Board to quantify device functionality; b) Pictures of the air pressure sensor on an alto (left) and tenor (right) saxophone.
During data collection, the patient was asked to sustain a 'G' note for as long as possible in one breath while duration and air pressure differentials were recorded by the sensor. Duration of note sustain was measured in seconds while pressure differentials were measured from the difference in air pressure between leads 1 and 2 in the mouthpiece. Videos of the patient playing with and without the embouchure-assistive device were recorded. Qualitative analysis of the patient 's performance was assessed by two experienced saxophone musicians. The patient was also interviewed after use of the device to obtain a subjective impression.
4. Results
3D scans of the patients face with KIRI engine and dental molds of the patient's embouchure confirmed that the area of air leakage was localized to the left oral commissure of the patient. Thus, the device was designed to seal and apply adequate supportive counter-pressure to this specific location, while minimizing skin contact for comfort.
The device increased the duration of time the patient could sustain the 'G' note by 68.3%, from 5.61 seconds without the device to 9.44 seconds with the device, as shown in Figure 7. On air pressure testing, The device also enabled a 39.6% increase in average air pressure that was directed into the mouthpiece, from 14.99 Pa without use of the device to 20.93 Pa with use of the device, as shown in Figure 8.
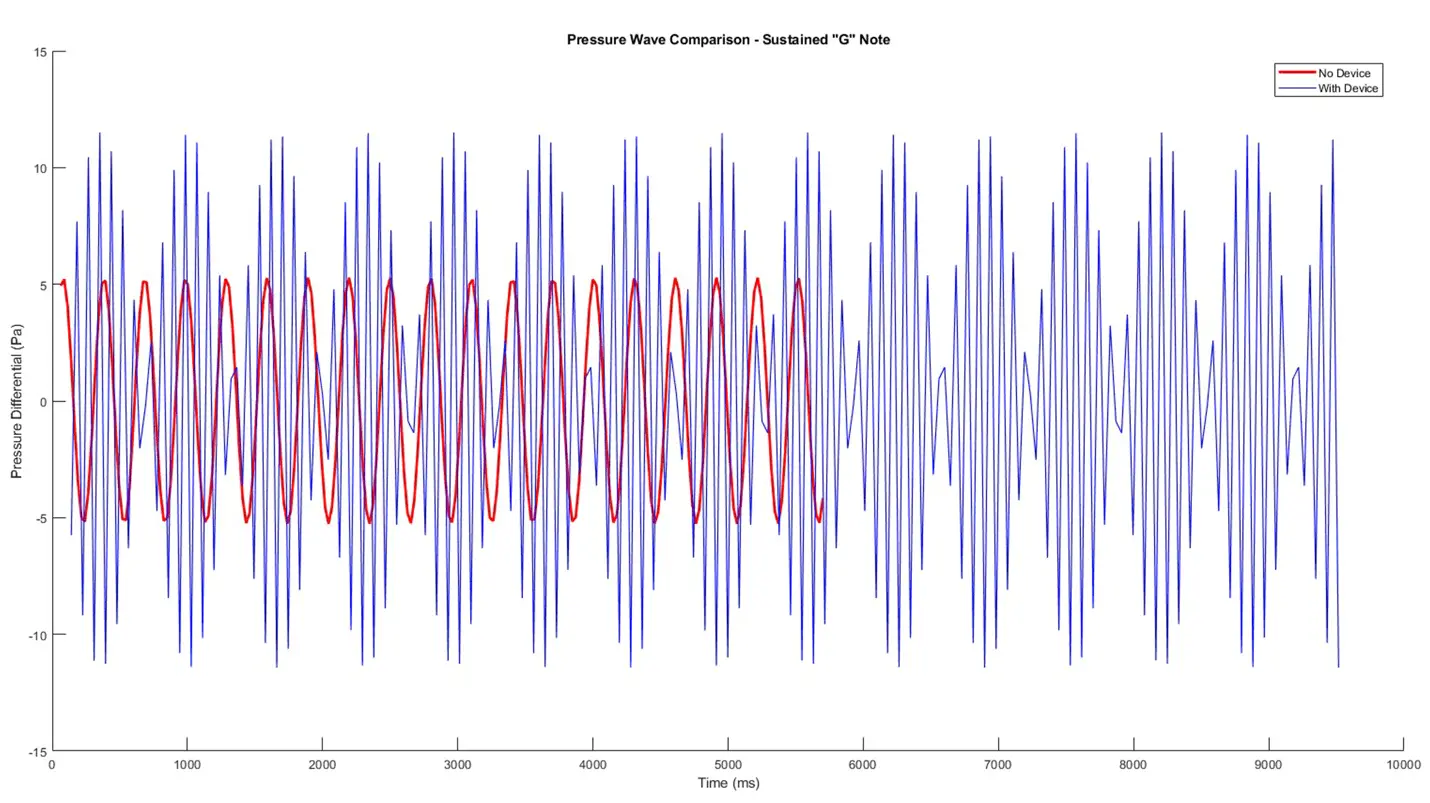
Figure 7. Pressure soundwave comparison exhibiting duration of 'G' note sustain with (blue) and without use of the device (red), depicting marked quantitative improvement in note sustain with the device.
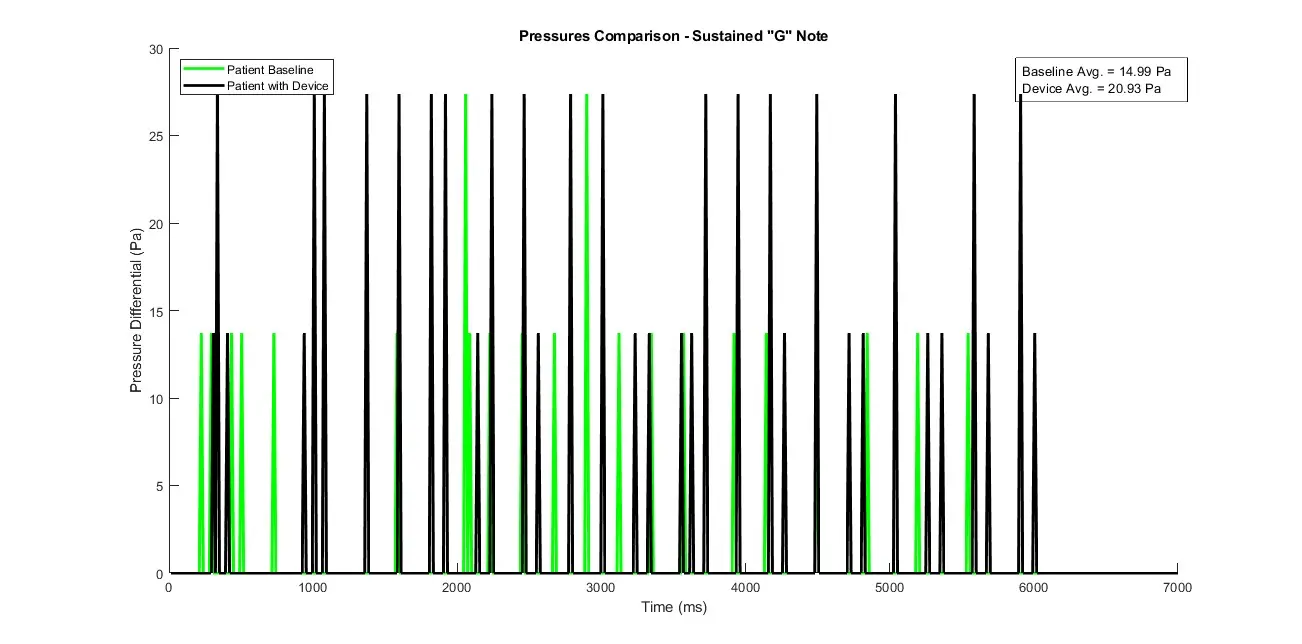
Figure 8. Patient air pressure differential through mouthpiece with (black) and without (green) use of the device, depicting showing marked quantitative improvement in air pressure with the device.
Qualitative analysis of the patient's playing revealed a substantial improvement in playing ability, quality, tone, and note sustain between playing without the device (Media S1) as compared to playing with the device (Media S2). Subjectively, the patient reported that the device helped him lose much less air while playing and effectively allowed him to create and maintain a seal with the mouthpiece and play louder, smoother, and longer. He reported that the silicone interface was soft and comfortable against his skin and helped form a malleable surface to better seal the areas of air leakage along his embouchure.
5. Discussion
The effects of facial palsy on activities of daily living are well-described and are commonly cited to impact speech, eating, and facial expression[2]. However, the effects of this condition on music production are not often documented. In the present study, we describe an inexpensive, 3D printed embouchure-assistive device that is functional, comfortable, and effectively restores a musician's ability to play their instrument after facial palsy. The device helped the musician create an airtight seal for maximum input airflow, strengthened pressure measurements, improved sound quality and performance, and increased duration of single note production. This device is reproducible using a 3D printer and the described materials for less than $6 and can be modified for general use across all woodwind instruments (Table S2).
The importance of embouchure for the woodwind player cannot be understated. This mechanism controls the dynamic airflow into the instrument, allowing for modulation of all the sound produced including pitch, volume, tone, timbre, and articulation[15]. Thus, facial palsy drastically impairs a musician's ability to produce sound and create music with their unique stylistic interpretation. An effective embouchure-assistive device for facial palsy requires sufficient support to maintain adequate airflow into the mouthpiece without leakage while still allowing for vibration of the reed[16]. Prior to this study, there have been only limited interventions to help musicians with facial palsy resume playing their instruments[17-19]. The design implemented in this study builds upon these concepts previously published online and in the literature.
There have been minimal embouchure assistive devices that have been built thus far. In a case report of a 47-year-old professional clarinet player with Bell's palsy, Aita-Holmes et al. utilized full-head 3-D imaging stereophotogrammetry to develop an assistive extraoral device clamped to the instrument[17]. The device pulls back the angle of the mouth, providing similar function as the buccinator muscle would. The patient reported satisfaction with the device, however, the authors note that the device was large, aesthetically unappealing, and made with expensive materials to which were molded to specifically and exclusively fit their patient's face. To address these drawbacks, our device was designed with reproducibility, cost-efficiency, and generalizability in mind, such that any musician with access to a 3D printer might be able to easily and inexpensively assemble this device for themselves.
In 2002, Gunnar Mossblad, professor of music at the University of Toledo, wrote an article in the Saxophone Journal about his experience with Bell's Palsy[18]. He created an external mechanical device, comprised primarily of metal spoons and rubber shoe soles, which attached to his mouthpiece and provided support to his cheeks and lips. However, Mossblad highlighted concerns for device stiffness and reported that occasionally his lips bled while playing. Our current design addresses these concerns by utilizing a thick silicone cushion that was soft enough to provide comfort and to fill in gaps between the device and the patient's embouchure. These factors were critical to our device design process to minimize pressure injuries, which can cause necrosis and ulceration.
While the embouchure-assistive device described supports the muscles of the face via external pressure, developments in the surgical management of facial nerve paralysis offer insight into potential future therapeutic alternatives to improve quality of life in patients with this condition[20]. Dynamic reanimation with gracilis free-muscle transfer allows for acceptable recreation of social smile. Improvements upon this concept have included double- and multi-paddle flaps, as well as dual-innervation to improve control of the muscle flap with acceptable results for smile outcomes[21-24]. In addition to free-muscle transfer, attempts at reanimation of the paralyzed face has expanded into the fields of materials science and electrical engineering. Developed by SRI International research laboratory, artificial muscle comprised of dielectric elastomers stretch in response to high-voltage current[25]. This has been studied in models of facial paralysis with promising results, however it has yet to undergo human trial due to high voltage requirements being incompatible with in vivo implantation[26-28]. Neuroprostheses are a developing field wherein electromyography signal from the contralateral face is fed to a processing unit, then used to drive firing of the impaired or implanted muscles of the paralyzed hemiface[29,30]. These designs offer an innovative approach to management of facial paralysis and may advance to support control of embouchure for musicians with facial palsy.
There are several limitations of this study as a case report of a prototype device. The device was designed to assist a specific patient with non-flaccid facial paralysis while playing the tenor saxophone and was not validated across a control, with other patients, or other instruments. The subject of this study had unilateral facial weakness and had an extensive surgical history with attempted dynamic reanimation, resulting in weak but present resting tone in his muscles of embouchure. As such, broad application to other patients with different levels of facial function may be limited; the device may not be as effective for patients with complete flaccid facial paralysis, soft tissue defects of the lips or face, or bilateral facial paralysis. Despite this, the malleable and adjustable soft facial apparatus may be modified to fit a variety of face shapes and support a range of embouchure deficiencies. Future studies will focus on modifying the device dimensions and validating the device across different severities of facial paralysis and across different woodwind instruments. Additional limitations within the design include the use of a hose clamp and zip-ties. These allowed for adjustability and accessibility within the specific test case but detracted from design aesthetics and reproducibility. Further study can focus on revision and implementation of an adjustable and reusable clamp system in lieu of zip-ties and a hose clamp. Lastly, future studies on embouchure-assistive devices should include validated metrics on quality of life, device use, and acoustic analysis of produced sound.
6. Conclusion
Facial palsy can have a profound psychological and functional lifelong impact upon the afflicted patient. In the case of woodwind instrumentalists, facial palsy may prevent formation of a proper embouchure and thus lead to inability to play. In this study, a 3D printable open-source embouchure-assistive device was designed and shown to effectively, safely, and comfortably support saxophone playing in a patient with facial palsy.
Supplementary materials
The supplementary material for this article is available at: Supplementary materials.
Acknowledgements
The author(s) would like to express immense appreciation to Mr. Peter Hergesheimer, the subject of the present case study, for his contribution, participation, and feedback in perfecting project design. The author(s) would also like to thank the UCSD Jacobs School Department of Mechanical and Aerospace Engineering (MAE) 156B Student Design Project.
Authors contribution
Brown D, Collier M: Devised methodology, engineered all iterations of this device, contributed conceptual design iteration of the device, collected and curated the data, analyzed the data.
Guzman C, Resendiz M: Devised methodology, engineered all iterations of this device, contributed conceptual design iteration of the device, collected and curated the data.
Saha I: Contributed conceptual design iteration of the device, contributed to supervision of the study, collected and curated the data, analyzed the data, drafted and edited the manuscript.
Greene JJ: Contributed conceptual design iteration of the device, contributed to supervision of the study, collected and curated the data, drafted and edited the manuscript.
Soliman SI: Analyzed the data, drafted and edited the manuscript.
Bernstein JD: Drafted and edited the manuscript.
All authors approved the final manuscript and offered feedback before publication.
Conflicts of interest
The authors declare no conflicts of interest.
Ethical approval
Institutional review board approval was obtained from the UCSD Human Research Protections Program (Project # 210007X).
Consent to participate
Informed consent was obtained from the patient participant prior to commencing the study.
Consent for publication
Consent for publication was obtained as part of written informed consent with the patient participant prior to commencing the study, and again when the manuscript was submitted for publication.
Availability of data and materials
The data and materials could be obtained from the corresponding author.
Funding
None.
Copyright
© The Author(s) 2023.
References
-
1. Walker NR, Mistry RK, Mazzoni T. Facial Nerve Palsy. Treasure Island (FL): StatPearls Publishing; 2023.[PubMed]
-
7. Schuele S, Lederman RJ. Focal Dystonia in Woodwind Instrumentalists: Long-term Outcome. Med Probl Perform Art. 2003;18(1):15-20.[DOI]
-
9. Fletcher N, Rossing T. Detailed Discussion of a Reed Generator. In: Fletcher NH, Rossing TD, editors. The Physics of Musical Instruments. New York: Springer Science & Business Media; 2008.
-
11. Steck D, Qu J, Kordmahale SB, Tscharnuter D, Muliana A, Kameoka J. Mechanical responses of Ecoflex silicone rubber: Compressible and incompressible behaviors. J Appl Polym Sci. 2019;136(5):47025.[DOI]
-
17. Aita-Holmes C, Liacouras P, Wilson WO Jr, Grant GT. Digital capture, design, and manufacturing of an extraoral device for a clarinet player with Bell's palsy. J Prosthet Dent. 2015;114(2):297-300.[PubMed]
-
18. Mossblad G [Internet]. Overcoming Bells-Palsey [cited 2023 Aug 20]. Available from https://gunnarmossblad.com/home/wp-content/uploads/2015/10/Overcoming-Bells-Palsey.pdf
-
19. Swampcabbage. Tools for facial paralysis and playing the saxophone [Internet]. Sax on the web.net; 2011 [cited 2023 Aug 20]. Available from: https://www.saxontheweb.net/threads/tools-for-facial-paralysis-and-playing-the-saxophone.157990/
-
21. Davis ME, Greene JJ. Advances and future directions in the care of patients with facial paralysis. Oper Tech Otolayngol Head Neck Surg. 2022;33(1):60-71.[DOI]
-
28. Konstantinidi S, Imholz C, Martinez T, Benouhiba A, Walter A, Civet Y, et al. Real-time actuation of a dielectric elastomer actuator neuroprosthesis for facial paralysis. Smart Mater Med. 2024;5(1):15-23.[DOI]
Copyright
© The Author(s) 2023. This is an Open Access article licensed under a Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, sharing, adaptation, distribution and reproduction in any medium or format, for any purpose, even commercially, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Publisher’s Note
Share And Cite




